
Navigating Postural Orthostatic Tachycardia Syndrome (POTS) & Dysautonomia
Living with Postural Orthostatic Tachycardia Syndrome (POTS) can feel like your body is stuck in a "fight-or-flight" storm that you didn’t ask for.
If you’ve been told your symptoms are "just anxiety," or if traditional talk therapy hasn't quite reached the physical intensity of your experience, you are in the right place.

What is POTS?
POTS is a form of dysautonomia—a malfunction of the Autonomic Nervous System (ANS). The ANS is the autopilot of your body, controlling things you don't think about, like blood volume & circulation, heart rate, blood pressure, and digestion.
In a regulated body, standing up triggers a quick adjustment to keep blood flowing to the brain. In a body with POTS, this handshake between the brain and the heart fails. Blood pools in the lower limbs, the heart overcompensates by racing, and the nervous system floods the body with stress hormones (such as adrenaline and norepinephrine) to keep you upright.
The result is a cluster of symptoms such as:
Tachycardia: Heart racing or palpitations upon standing.
Orthostatic Intolerance: Dizziness, lightheadedness, or fainting.
The Invisible Toll: Brain fog, profound fatigue, tremors, "air hunger”
This brief list doesn't nearly capture the full range and severity of ways POTS can affect an individual's life.

Who Gets POTS?
While historically diagnosed most commonly in childhood and adolescence (predominantly in girls and those assigned female at birth) we now know that POTS can affect anyone, of any age.
It is often triggered by a major "system shock" such as:
Viral or bacterial infections.
Concussions or physical trauma.
Pregnancy or major surgery.
Puberty and hormonal shifts.

The Post-COVID Influx
The landscape of POTS changed dramatically following the COVID-19 pandemic. Current 2025/2026 data indicates that approximately 1 in 3 Long COVID patients meets the diagnostic criteria for POTS. The virus acts as a potent trigger for the neuroimmune axis, causing a "stuck" sympathetic nervous system response that persists long after the initial infection has cleared.
POTS rarely travels alone. We now recognise a trifecta (and sometimes a quadfecta) of conditions that often co-occur:
Neurodivergence (ADHD & Autism): There is a significant correlation between hypermobile bodies (EDS) and neurodivergent brains. Research suggests that a highly sensitive nervous system may be more prone to autonomic dysregulation.
Autoimmune Conditions: Emerging research (2025) has identified specific G-protein coupled receptor antibodies in POTS patients, suggesting that for many, POTS is a neuroimmune disorder rather than a simple cardiovascular one.
Hypermobility (hEDS): Many POTS patients have stretchy connective tissue, which allows blood vessels to expand too easily, leading to the "pooling" that triggers the heart rate spikes.
The Intersection: Neurodivergence & Autoimmunity

The Roadmap to Management: A Whole-Body Approach
Effective POTS care is rarely about just one thing. According to the 2025 Australian POTS Registry—the largest study of its kind in Australia—successful management requires a "biopsychosocial" framework.
Why a Multi-Disciplinary Team is Essential
The Registry data highlights why specialised, integrated care is so important for the Australian patient:
The Diagnostic Gap: On average, it takes 5.8 years for an Australian to receive a POTS diagnosis.
The Misdiagnosis Hurdle: 64% of patients were initially told their symptoms were "purely psychiatric" (like anxiety) before their POTS was correctly identified.
The Gold Standard Medical Pathway
Standard medical management typically follows a four-stage process, as outlined in current clinical guidelines:
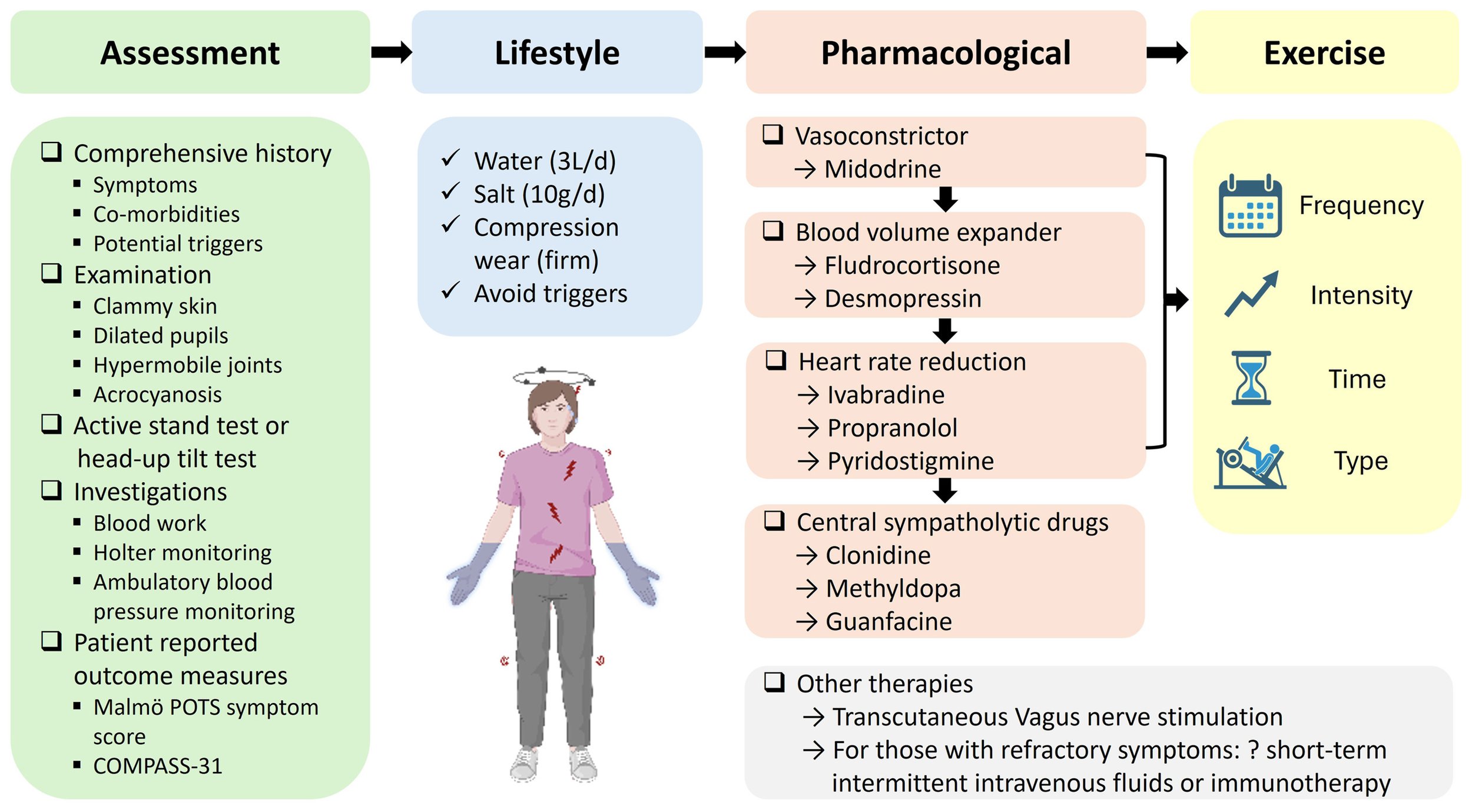
Source: Heart, Lung and Circulation (2025). Reproduced from Butler et al., "Postural Orthostatic Tachycardia Syndrome: A Review of the Australian Experience and Registry Data." View full study here.
Why Psychology is a Vital Piece of the POTS Puzzle
Managing POTS is often described as fixing the body’s "plumbing" (blood volume) and "electricity" (heart rate). While these medical treatments are essential, they sometimes miss the "operating system" that runs it all: your Autonomic Nervous System (ANS).
For many living with POTS, the nervous system becomes stuck in a state of high alert (hyperarousal). This isn't just a feeling; it is a physical change in how your brain processes signals from your body.
This is why psychology and somatic therapies are not "alternatives" to medical care—they are the bridge that makes medical care more effective.

Why "Talking About It" Isn't Enough
If folks with POTS are referred at all for therapy, it is often with a diagnosis of anxiety. While living with POTS is undoubtedly anxious-making, the anxiety is often a result of the physiology, not the cause of it.
Traditional Cognitive Behavioral Therapy (CBT) focuses on "top-down" processing - changing your thoughts to change your feelings.
However, if your heart is beating at 130bpm while you are just standing at the kitchen sink, challenging your thoughts won't stop the physiological flood of adrenaline.
As Dr Russell Kennedy so eloquently describes in his powerful book Anxiety Rx (link here) - “you can’t think your way out of a feeling problem”.

How the Northground approach can help……


The Power of Somatic Regulation
Standard talk therapy focuses on your thoughts. However, POTS is a physiological storm that often resists logic. You can't "think" your way out of a racing heart or a dizzy spell.
That’s why we use "Bottom-Up" Somatic Therapies (such as EMDR, EFT/Tapping, and Somatic Experiencing). Instead of just talking, these methods work directly with the brainstem and the nervous system to:
Calm the "Smoke Detector": Help the brain (specifically the insular cortex) stop overreacting to internal body signals.
Lower Stress Hormones: Research shows tools like EFT (Tapping) can reduce cortisol by up to 37% and improve heart rate variability (HRV).
Rewire the Habit of Arousal: Help your body "unlearn" the state of constant fight-or-flight that chronic illness creates.
How this helps you:
Better Symptom Stability: A calmer nervous system supports your medication and physical rehab.
Reduced "Body Vigilance": Learning to trust your body’s signals again.
Comprehensive Care: Treating the person, not just the pulse
You don't need a therapist to tell you your symptoms are in your head. You need a clinician who understands the neurobiology of dysautonomia and can help you build a "manual" for your unique nervous system.
If you are looking for a biopsychosocial approach that honours your physical reality while providing somatic tools for recovery, we would love to support you.
In the meantime, feel free to dive into our POTS Resource Hub for more tools and guides
Clinical References
Australian POTS Foundation Registry. (2025). Symptom burden, quality of life, and diagnostic journey of people with POTS, Australia, 2021–24. Medical Journal of Australia.
Boris, J. R., Shadiack, E. C., McCormick, E. M., MacMullen, L., George-Sankoh, I., & Falk, M. J. (2024). Long-term POTS outcomes survey: Diagnosis, therapy, and clinical outcomes. Journal of the American Heart Association, 13(2).
Csecs, J. L., et al. (2022). Joint Hypermobility Links Neurodivergence to Dysautonomia and Pain. Frontiers in Psychiatry.
Davis, H. E., et al. (2023). Long COVID: Major findings, mechanisms and recommendations. Nature Reviews Microbiology.
Dolphin, H., et al. (2022). “The wandering nerve linking heart and mind”: The complementary role of transcutaneous vagus nerve stimulation in modulating neuro-cardiovascular and cognitive performance. Frontiers in Neuroscience, 16.
Eccles, J. A., et al. (2024). The neurobiology of the 'Pentad': Hypermobility, POTS, MCAS, Neurodivergence, and Gastroparesis. Journal of Personalized Medicine.
Porges, S. W. (2021). Polyvagal Safety: Attachment, Communication, Self-Regulation. W.W. Norton & Company.
Seeley, M. C., et al. (2026). Postural Orthostatic Tachycardia Syndrome: A State-of-the-Art Review. Heart, Lung and Circulation.
Stapleton, P., et al. (2025). How tapping works: Physiological and psychological mechanisms in energy psychology treatments. Frontiers in Psychology.
Umeda, S., Harrison, N. A., Gray, M. A., Mathias, C. J., & Critchley, H. D. (2015). Structural brain abnormalities in postural tachycardia syndrome: A VBM-DARTEL study. Frontiers in Neuroscience, 9.
University of Adelaide / SAHMRI. (2025). Reduced cerebral blood flow and its relationship to sensory processing in POTS. Scientific Reports.
Vernino, S., et al. (2024). Postural Orthostatic Tachycardia Syndrome: Clinical presentation, etiology, and management. Mayo Clinic Proceedings.


